Setting Up A Pathway to Improve Management of Cognitive Impairment in People With MS Using Screening With The Symbol Digit Modality Test Prior To Referral To Neuropsychology
Poster
Project write up
Introduction
Cognitive impairment is a common problem associated with multiple sclerosis (MS) and is reported to occur in around one third of people with MS (pwMS) at diagnosis increasing to 50% by 5 years (Reuter et al, 2011). Rates are reported to vary according to clinical subtype including; 35% of those with clinically isolated syndrome (CIS), 45% of those with relapsing-remitting MS (RRMS), 79% of those with secondary progressive MS (SPMS) and 91% with primary progressive MS with an average prevalence of 46% cross all pwMS (Ruano et al, 2017). These rates suggest that cognitive impairment worsens with disease progression. CI may also acutely worsen during an MS relapse (Benedict et al, 2020), with incomplete recovery contributing to 10-year disability in patients with RRMS (Sotiropoulos et al, 2021).
Cognitive domains affected include learning and memory (including immediate and delayed recall, recognition and prospective memory), attention, concentration, mental speed, problem solving and word finding difficulties (Rouleau et al., 2018). As a result, many aspects of an individual’s life are impacted including ability to work, socialise and to carry out everyday tasks. Cognitively impaired pw MS report loss of self-esteem and independence, impaired family life, impaired social relationships, sexual dysfunction and higher rates of divorce.
CI may also result in reduced engagement with the MS MDT resulting in poor compliance with medical therapies which can result in loss to follow up. Ultimately, CI can have implications for the individuals’ capacity to make decisions according to the Mental Capacity Act (2005) thereby reducing autonomy.
Issues with Management of CI
Cognitive Impairment often coexists with, and is impacted by, other symptoms common in MS such as fatigue, mood disorders and pain (Hansen & Lautenbacher, 2017). Therefore comprehensive symptom management is necessary as recommended in The NICE guidance for the management of Multiple Sclerosis. NICE suggest that these issues can be addressed through support by a clinical neuropsychologist. However, no formal care pathways for pwMS with anxiety, depression and CI exist locally or nationally and access to clinical neuropsychology is limited, with inequity between geographical locations.
For example, in many regions associated with DGHs, such as Surrey Downs Health and Care (SDH&C), access to clinical neuropsychology is limited. There is currently only a 0.44 whole time equivalent (WTE) clinical neuropsychologist in the SDH&C multidisciplinary community neurorehabilitation team. As a result, their clinical support is only available to individuals with acquired brain injuries and functional neurological conditions and not for progressive neurological conditions such as MS. In fact, there is currently no specific neuropsychology funding for pwMS with CI despite its prevalence, impact on quality of life and economic impact to a) the patient (loss of income as they will leave work early due to undiagnosed CI), and b) to the NHS, which is significant and growing (Neurological Alliance report 2021).
The current pathway for formal cognitive assessment is to refer patients to the MS neurology service in the regional neurosciences centre at St. George’s Hospital, London who in turn refer to their neuropsychology team. This process results in delayed assessment whilst moving patients unnecessarily into secondary care. Whilst this service provides comprehensive assessment, it serves a wide geographical area and therefore waiting times can be variable and travel times can be an issue, especially for pwMS with disability and fatigue. Moreover, the communication of results to the local MS team is variable and for the majority, little ongoing care or management strategies are offered once assessments are completed.
A further issue that can interfere with instigating appropriate cognitive assessment is that pwMS with CI often have reduced insight into their difficulties affecting subjective self-reporting of issues. Therefore, CI may only be detected once it is at a relatively advanced stage at which point management strategies may be harder to institute.
A potential solution to tackle these issues would be for the local MS team to routinely incorporate valid and reliable cognitive assessment into their annual patient review to allow early identification of cognitive issues as well as any progression over time.
One such measurement tool is the Symbol Digit Modality Test (SDMT) from the Brief International Cognitive Assessment for Multiple Sclerosis (BICAMS), established through an international expert consensus committee (Benedict et al, 2012), with evidence supporting its sensitivity and specificity as a screening tool (Benedict et al., 2017; Corfield & Langdon, 2018; Artemiadis et al, 2021).
Establishing a baseline cognitive assessment score would promote early identification of cognitive decline as well as facilitating monitoring of cognition over time in an objective and reproducible manner. The hope is that this will aid early identification of pwMS who may need more comprehensive neuropsychological input, including measurement and management strategies.
Aim
The aim of this project is to establish the feasibility and utility of using the SDMT for cognitive screening at diagnosis and follow up in pwMS with a view to setting up a standardised pathway for formalised cognitive assessment across the region.
Objectives
- To identify the associated material costs, training requirements and impact on workload as well as support required from a clinical neuropsychologist to perform cognitive screening tests.
- To identify the prevalence of Cognitive impairment (CI) in people with MS (pwMS) across the Surrey Region and how this screening tool can monitor how this may change over time.
- To identify suitable cut-off values to trigger onward referral.
- To identify the level of unmet need for neuropsychology input for pwMS and to help develop a business case for this across SDH&C
- To co-ordinate MS services in Surrey, to allow development of standardised pathways for assessment and management of CI with a view to influence local and national pathways.
Methods
100 pwMS (of varying diagnoses and stage) from 4 MS centres across Surrey and South London will be asked to complete the SDMT at their clinic appointment under the supervision of an MS clinician (nurse or doctor). Patients will also be asked to complete a baseline characteristics form, a mood screening questionnaire (HADS / PHQ+GAD), and a pain questionnaire if indicated.
Training will be provided by Dr Seb Potter, Consultant Clinical Neuropsychologist, Surrey Downs Health & Care and further advice will be sought from University departments at Nottingham and Roehampton from researchers who have been developing cognitive screen measures and/or investigated their implementation in clinical settings.
Results
At this time we have been working to set up a proposed pathway to map the use of the SDMT to assess cognition in our patients ad onward referral. We have also established participating MS centres to carry out the audit and have attained the materials needed as detailed below:
The journey so far…
October 2019 – Pathway mapping steering group meeting – Lack of Neuropsychological support for patients with suspected Cognitive Impairment identified
Jan 2020 – Findings presented to St George’s regional MS MDT education meeting
March 2020 – Covid19 pandemic isolates pwMS and limits access to MS services. No visual assessments possible & all other contact limited due to short staffing
Sept 2021 – Advanced MS Academy Masterclass delegate – subject for project agreed
Sept 2021 – Meeting with Dr Seb Potter, Neuropsychologist, keen to be involved
Sept 2021 – Surrey MS Practitioner meeting Ruth presents idea for audit, group agreement
Sept 2021 – Application to Novartis to fund 4 licenses = 100 assessments, successful
Sept 2021 – Initial mapping meeting for an ‘Anxiety, depression and CI pathway’ for SDH&C
October 2021 – Follow up meeting to update pathway
Dec 2021 – Surrey MS Practitioner meeting- Ruth Stross & Seb Potter present work so far
Dec 2021 – Follow up meeting to update pathway
Dec 2021 – Patient audit questionnaire draft completed, pack with include HADS & MFIS - 5
Jan 2022 – Discussion re Surrey audit to include St George’s (Regional MS Centre)
Jan 2022 – Despite regular emails to the NHS Trust finance team the funding has not been brought across so the SDMT has not been purchased. Funding almost lost due to this delay
10 Feb 2022 – Surrey MS practitioner meeting – training on SDMT, feedback on questionnaire &
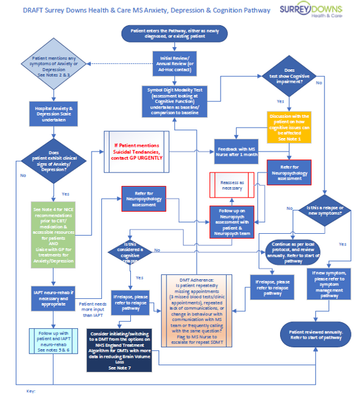
The Proposed Pathway
Summary
Cognitive Impairment is a significant issue in pwMS and is currently under reported and poorly managed. This project aims to establish the use of a cognitive screening tool as standard practice in our local region with a view to standardising pathways for access to neuropsychological services.
The next step is to start the audit, gather and analyse the data, disseminate the information and formalise the plan for our regional pathway.
References
Artemiadis A, Bakirtzis C, Chatzittofis A, Christodoulides C, Nikolaou G, Boziki MK, Grigoriadis N. (2021) Brief international cognitive assessment for multiple sclerosis (BICAMS) cut-off scores for detecting cognitive impairment in multiple sclerosis. Mult Scler Relat Disord. Apr;49:102751.
Benedict RHB, Amato MP, DeLuca J, Geurts JJG. (2020) Cognitive impairment in multiple sclerosis: clinical management, MRI, and therapeutic avenues. Lancet Neurol. Oct;19(10):860-871Benedict, R. H., et al. (2017). Validity of the Symbol Digit Modalities Test as a cognition performance outcome measure for multiple sclerosis. Multiple Sclerosis Journal, 23(5), 721–733.
Benedict, RH et al., (2012). Brief International Cognitive Assessment for MS (BICAMS): international standards for validation. BMC Neurol Jul 16;12:55.
Corfield F, Langdon D. A Systematic Review and Meta-Analysis of the Brief Cognitive Assessment for Multiple Sclerosis (BICAMS). (2018) Neurological Therapeutics. Dec;7(2):287-306.
Elwick H, Topcu G, Allen CM, Drummond A, Evangelou N, Nair RD. (2021) Cognitive measures used in adults with multiple sclerosis: A systematic review. Neuropsychol Rehabil. 2021 Jun 13:1-18. Hansen, S., & Lautenbacher, S. (2017). Neuropsychological assessment in multiple sclerosis. Zeitschrift Für Neuropsychologie, 28(2), 117–148.
Morrow SA, O'Connor PW, Polman CH, Goodman AD, Kappos L, Lublin FD, Rudick RA, Jurgensen S, Paes D, Forrestal F, Benedict RH. (2010) Evaluation of the symbol digit modalities test (SDMT) and MS neuropsychological screening questionnaire (MSNQ) in natalizumab-treated MS patients over 48 weeks. Mult Sclerosis. Nov;16(11):1385-92.
Neurological Alliance report 2021
Reuter F, Zaaraoui W, Crespy L, Faivre A, Rico A, Malikova I, Confort-Gouny S, Cozzone PJ, Ranjeva JP, Pelletier J, Audoin B. (2011) Cognitive impairment at the onset of multiple sclerosis: relationship to lesion location. Mult Sclerosis. Jun;17(6):755-8. Rouleau, I., Dagenais, E., Tremblay, A., Demers, M., Roger, É, Jobin, C., & Duquette, P. (2018). Prospective memory impairment in multiple sclerosis: A review. The Clinical Neuropsychologist, 32(5), 922–936.
Ruano L, Portaccio E, Goretti B, Niccolai C, Severo M, Patti F, Cilia S, Gallo P, Grossi P, Ghezzi A, Roscio M, Mattioli F, Stampatori C, Trojano M, Viterbo RG, Amato MP. (2017) Age and disability drive cognitive impairment in multiple sclerosis across disease subtypes. Mult Sclerosis. Aug;23(9):1258-1267.
Sotiropoulos MG, Lokhande H, Healy BC, et al. (2021). Relapse recovery in multiple sclerosis: Effect of treatment and contribution to long-term disability. Multiple Sclerosis Journal - Experimental, Translational and Clinical. Vol 7(2).
More MS Academy Service development Projects
Encouraging excellence, developing leaders, inspiring change
MS Academy was established in 2016 and in that time has accomplished a huge amount with exciting feedback demonstrating delegates feel inspired and energised along their personal and service development journeys. The various different levels of specialist MS training we offer are dedicated to case-based learning and practical application of cutting edge research.