Built on partnerships: we dig deeper into the Parkinson's Excellence Network
NewsLaunched in 2015, the UK Parkinson's Excellence Network began at an event in Leeds where healthcare professionals came together to formally recognise the strength that comes from sharing good practice, providing support and working to common goals.
Parkinson's Academy spoke with consultant geriatrician Professor Richard Walker, who has been with the Network from that first conference, and Rowan Wathes, Associate Director of the Excellence Network, to find out more about the Network's past and its focus today.
Prof Richard Walker
Initially identifying a handful of core areas to focus on - including Richard's own group looking at under-served communities within Parkinson's care - and launching working groups to address these needs, the grassroots Network has continued to grow to encompass Parkinson's specialists at every level.
Today, it is clear that the Network's core strength lies in its partnership mentality, and the impact that these partnerships can have at a national, regional and local level in effecting change and improving outcomes for people with Parkinson's.
Prof Richard Walker
Meaningful partnerships
The Network's current priorities have been identified using the recent 2019 Parkinson's UK audit, drawing on the amassed evidence across clinical practitioners and people affected by Parkinson's to inform the areas of greatest need (fig 1). These contribute to the delivery of the ‘Better support, every day’ theme of the Parkinson’s UK strategy.
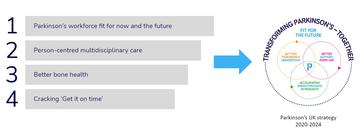
Figure 1: Parkinson's Excellence Network national programmes, taken from the PEN slideset
Whilst working closely with Parkinson's UK and able to draw on the evidence they gather, this is very much a partnership rather than an ownership, which sits squarely with healthcare professionals who volunteer their time and energy where needed, and who align their working goals with the Network's values.
Richard Walker
As with all partnerships, there is a benefit to both organisations, as Rowan shares clearly.
Rowan Wathes
Historically, the Excellence Network has pump-primed specialist nursing posts, but recently the network has also funded Parkinson’s practitioner posts and a Clinical and Research Fellowship in Cumbria (a region that has historically struggled to recruit medics).
The importance of partnership is highlighted further when viewed alongside the Network's underpinning principles, of which 'To involve people with Parkinson’s at every stage' is the first. Rowan explained how partnering with people with Parkinson's is integral to the work of the Network, and how individuals affected by Parkinson's have an equal role on the national steering groups and increasingly within regional networks, and in contributions at a local level.
Rowan Wathes
After a discussion of what meaningful involvement can look like and the importance of having involvement from people with Parkinson's who can take a broader view of the issues being addressed, Richard shared the incredible work done by Jane Rideout who lives with Parkinson's and led the Regional Network for the Southwest of England until recently. He also gave a clear example of how people with Parkinson's bring a unique perspective and understanding as well as an ability to communicate in ways that healthcare professionals cannot.
Prof Richard Walker
It can be difficult to find people who are both willing and able to partner with professionals to effect change, but Richard notes that 'proactive people often self-select themselves'. As an example, he spoke of Omotola Thomas, a younger woman with Parkinson's who is originally from Nigeria, and who has now contributed a great deal to the Parkinson's community as a spokesperson.
Prof Richard Walker
Local services, national improvement - sharing learning to instigate change
The grassroots initiative from healthcare professionals operates at three levels - national, regional, and local. With multiple disciplines involved at each level, information is shared both top-down and bottom-up, depending on what is most appropriate.
Prof Richard Walker
A local initiative might be shared at a regional meeting and then be featured at a national conference or in the Network's newsletter, whilst national evidence or guidance might be shared at a regional level and then used to implement change locally by individual teams. Any network is only as strong as its members and it is through partnership working that the Excellence Network can really benefit those with Parkinson's.
Bone health
One of the priorities of the network this year is bone health. Highlighted as an issue by the Parkinson's UK's 2019 audit, and known to be an issue clinically, the work around bone health has led to a national piece of work to develop a clear guidance framework for supporting bone health in Parkinson's in the form of a flowchart.
Rowan Wathes
The bone health improvement initiative highlights evidence that people with Parkinson’s are more than twice as likely to have osteoporosis and are twice as likely to have a fracture than those unaffected with 50% of fractures in Parkinson's hip-related. In addition, 50% of people with Parkinson’s report falling more than once during a 3-month period and 13% report falling more than once a week. Finally, the evidence shows that fractures are a major cause of emergency hospital admission for people with Parkinson’s, who are more than twice as likely to be hospitalised due to a hip fracture than those without Parkinson's.
Prof Richard Walker
Driving
Driving and Parkinson's is another area of care and support that can be challenging to manage well. Evidence on whether a person with Parkinson's can drive safely is self-reported, or relayed by a carer, and much of a person's safety around driving is to do with personal insight and good self-management.
Richard shared how meaningful it was to listen to people with Parkinson's at a national meeting as part of research into driving, noting that individuals shared insights into their condition and driving in an open and honest way, as perhaps they would not be likely to do in a consultation.
He highlighted the benefit of hearing how people manage themselves by driving in 'on' times, for example, or have an awareness of how their impulse control disorder leads to faster driving. This, coupled with people with Parkinson's hearing how a driving assessor aims to enable them to adapt whilst still keeping their independence, was helpful to everyone in the room.
The paper resulting from this work, when reviewed alongside recent driving assessment guidance which has come out of a working group in Wales, demonstrates the benefit of sharing local work at a national level, creating a combined body of evidence which can in turn improve working practice or patient outcomes.
More information
Find out more about the driving assessment questionnaire and guidance from the South Wales Parkinson's Nurse Specialist Group
Learn more about the Bone health initiative
Read the 2019 Parkinson's audit
Find out more about the recent 2021 Conference and awards
Visit the Excellence Network's learning hub
Sign up for the Excellence Network newsletter here
Read an interview with Omotola Thomas in the Journal of Parkinson's disease
Related articles
'The things you can't get from the books'
Parkinson's Academy, our original and longest running Academy, houses 23 years of inspirational projects, resources, and evidence for improving outcomes for people with Parkinson's. The Academy has a truly collegiate feel and prides itself on delivering 'the things you can't get from books' - a practical learning model which inspires all Neurology Academy courses.


