Neurology Network Manager's Meeting, May 2021: in summary
News
Georgina Carr, Prof Adrian Williams and Sue Thomas
On 12th May, over 80 delegates attended the second Neurology Network Manager's Meeting, delivered virtually through Neurology Academy's online learning space. All of the Faculty delivered their presentations and panel discussions live from a central venue whilst the app sli.do was used to encourage questions and participation from delegates.
The benefits of on-demand learning meant that there was flexibility in attending 'live' or catching up later. The result was an average of 50 attendees at any given time, with healthcare professionals, commissioners and providers attending for live sessions where possible and using Neurology Academy's online learning space to access other sessions at a convenient time to them.
Whilst the meeting addressed a wide range of topics, the key messages to come out were around:
a reduced workforce 'norm' after redeployed individuals have returned to reduced neurology hours,
the challenges of business planning and how we can demystify and upskill people in the art of business case writing
the importance of mental resilience for a positive and well-functioning team
the importance of gathering data from service users and how we can capture the lived experience of those with a neurological condition.
'The lost hours'
We know that neurology has been experiencing significant understaffing in recent years, highlighted by the MS services audit presented at Raising the Bar 2020, and in the recent MS report 'NHS Reset and Reform'.
We also know that a large number of specialist staff have been redeployed from their roles in neurology in the past year, with Neurology Academy surveys finding 54% of respondents had experienced reduced teams due to redeployments to general medicine, in response to the coronavirus pandemic.
Whilst these redeployments were entirely understandable, worryingly, a sli.do poll at the Neurology Network Managers meeting (Fig 1) found that 69% of previously redeployed respondents had found that staff returning to their original posts had less hours allocated to neurology than previously. Given the current backlog of patients awaiting routine appointments in neurology, this reduction of staff time will further impact the workforce's ability to 'catch up' - and add to the pressures on neurology teams.
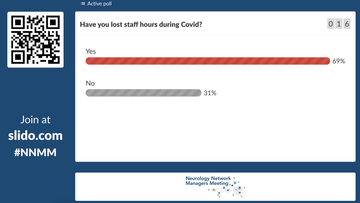
Fig 1: A sli-do poll during the meeting found 69% of respondents had lost staff hours on returning to their usual posts following COVID-related redeployment
Another challenge highlighted at the meeting around the NHS workforce was that of recruitment to specialist nursing posts. Reportedly, there is a lack of applicants for the essential posts, whilst applications are coming from therapy positions. These individuals, despite their own considerable specialties, often do not have the competencies needed for specialist nursing posts, placing additional demands on the workforce, services, and crucially, how individuals experience those services and manage their conditions.
The mystery of business planning
The meeting this May highlighted a very practical need - training and support in business planning, and specifically, in developing business cases. Feeling competent and confident in writing business cases can mean the difference between struggling in an existing service and feeling frustrated about it, and acting on changes that are needed to deliver an improved service in the future.
Dr Agne Straukiene, consultant neurologist and lead for 'Living well with MS'
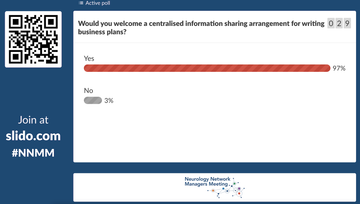
Fig 2: A sli-do poll during the meeting found 97% of respondents would welcome a toolkit or set of resources to support writing business case
As a direct result of the NNMM, a working group is being formed to create a toolkit of resources, available online, with both tips and information on how to write a good business case, templates to work from. The toolkit will also include example business cases for services that often require staff to write a business case such as MDT coordinator posts, administrative support, specialist nurse posts, and wellness clinics.

Fig 3: An example of the core questions to ask to identify service change - essential before writing any business case
Once developed, a practical webinar will be run live, and available on-demand, to support use of the toolkit, to give a clear overview of what, why and how to write, and to answer any questions.
Prioritising your own resilience
Prof Matthew Cripps, Director of Sustainable Healthcare, NHS England presented his experience of building resilience in his own team, both before and during the coronavirus pandemic, and how they used the concept of 'Team Happiness'.

Fig 4: Slide from Matthew Cripp's presentation - 'the key ingredients of Team Happiness'
Matthew spoke of the importance of making small changes which can have a big impact on a team's productivity, effectiveness, calmness and wellbeing, and offered to share an existing list of proven marginal gains with anyone who is interested. Ensuring that every individual within a team understands 'what to do and how to do it' is important, as is considering the five elements which lead to 'Team Happiness' including kindness, EDI - equality, diversity and inclusion, wellbeing, process engineering, and a flat thinking hierarchy.
Matthew has kindly given permission to share his presentation, which was incredibly well received.
Encouraging better data
The need for more - and better - data is a regular discussion, and Neurology Network Managers heard from Georgina Carr, CEO of the Neurological Alliance, about how the new app NeuroLifeNow is gathering meaningful data from people living with neurological conditions. However, the more app users, the more data is gathered, and the more meaningful that data becomes.
Georgina encouraged healthcare professionals to encourage people living with neurological conditions to sign up to the app (also available in a web browser for those without Smart devices) and to complete the monthly surveys. The better understanding of people's experiences and access to neurology services and support that this data could provide is invaluable.

Related articles
Meet with strategic and operational colleagues in neurology
Join us for the Neurology Manager Network Meeting which will enable senior managers and directors in neurology services to update their knowledge on current neurology service delivery.


